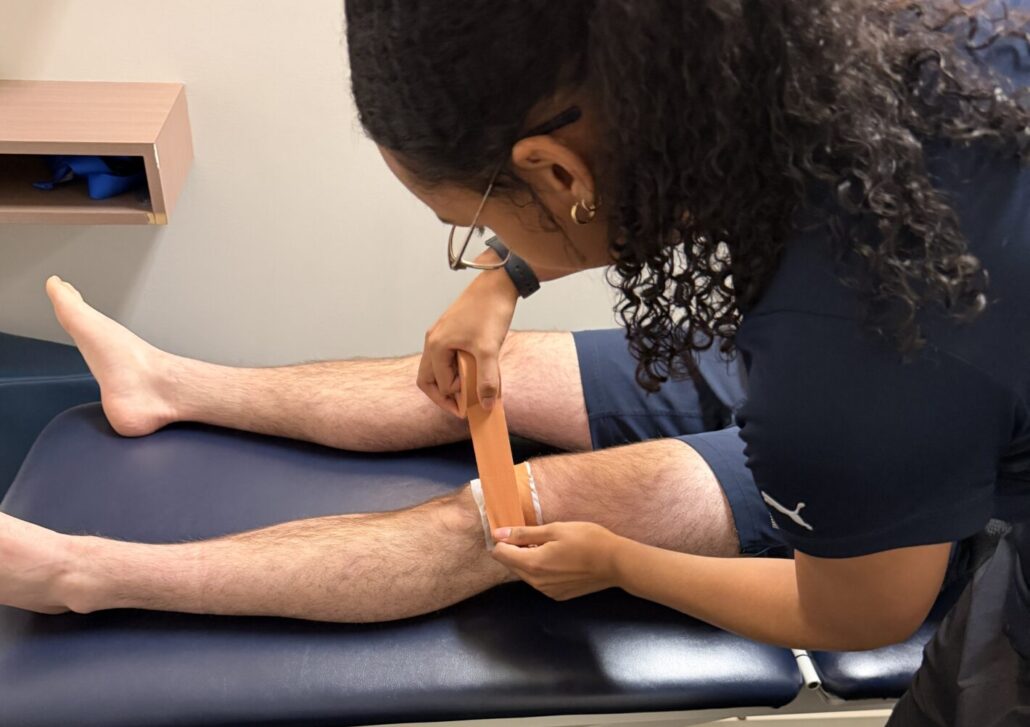
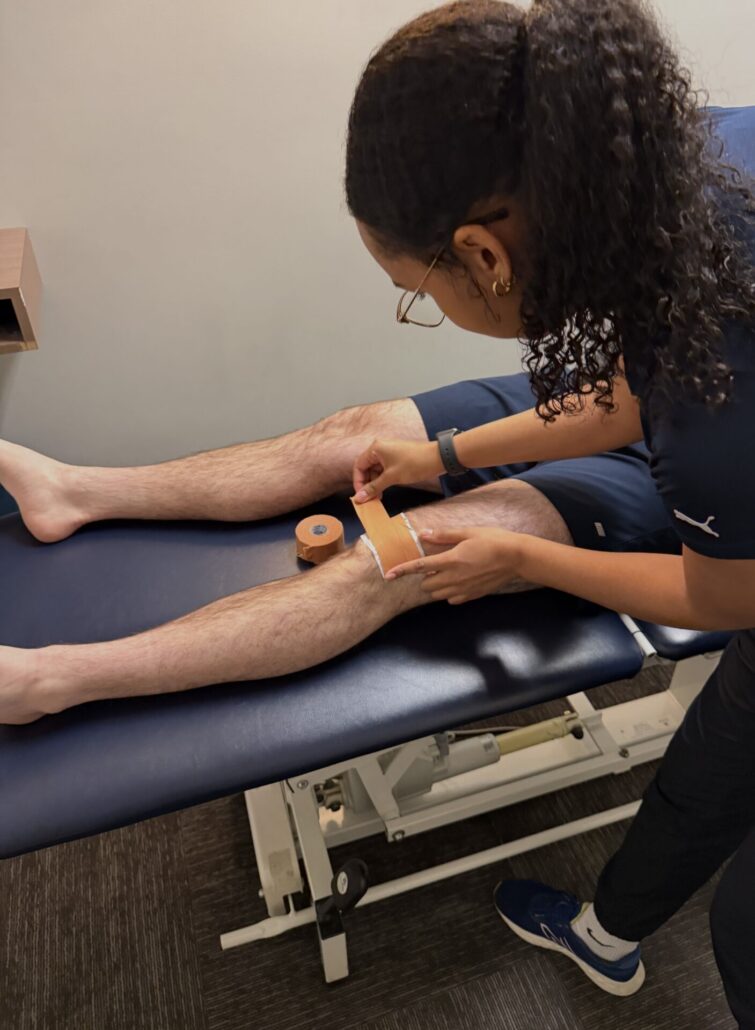
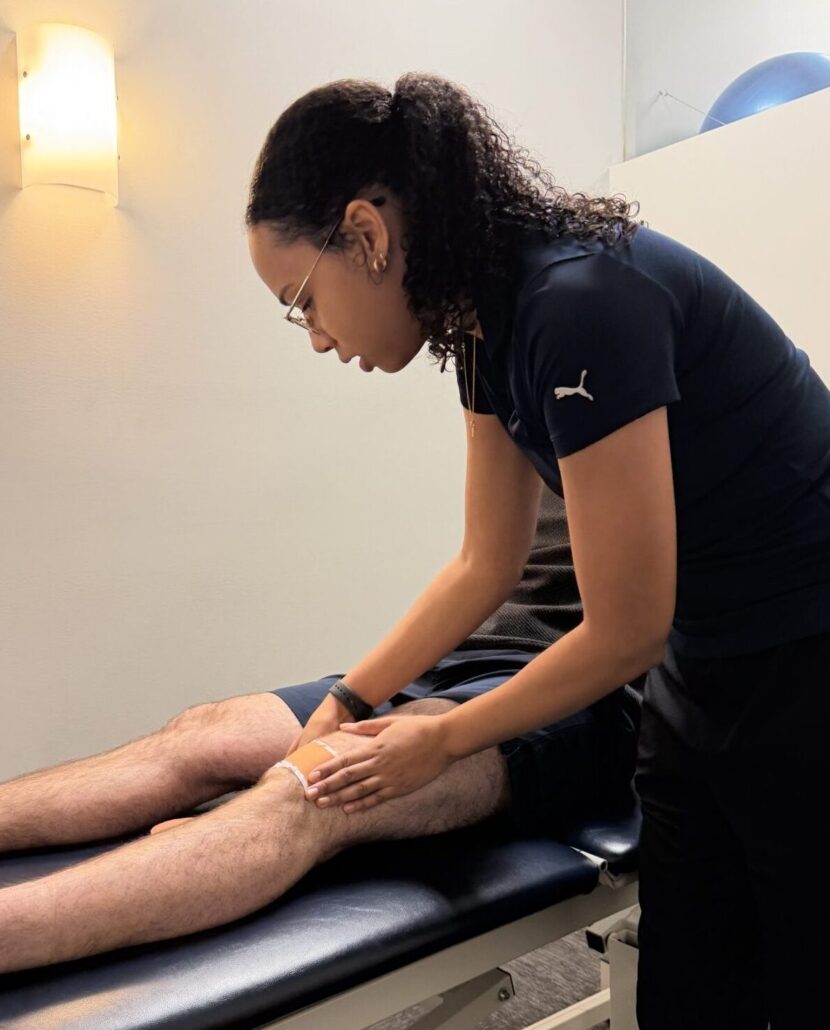
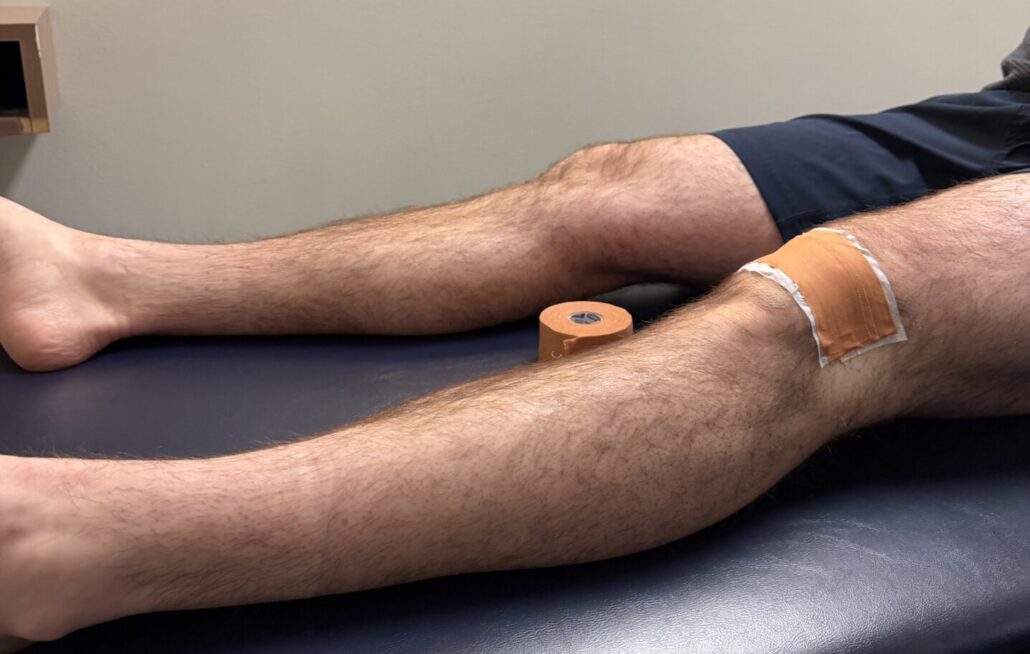
How Your Pelvic Floor May Be Impacting Your Postpartum Health

TL;DR
Your pelvic floor affects more than bladder control after childbirth. Symptoms like persistent lower back pain, pelvic pressure, painful intimacy, and bowel changes often signal pelvic floor dysfunction, not just “normal” postpartum recovery. Early pelvic floor physiotherapy assessment helps identify these connections and supports comprehensive healing.
───────────────────────────────────────────
The months following childbirth bring tremendous physical changes, and many new mothers experience symptoms they assume are simply part of recovery. While some discomfort is expected, certain signs often dismissed as “normal” postpartum changes may actually indicate pelvic floor involvement.
Understanding these connections helps you recognize when professional support might benefit your recovery. The pelvic floor plays a central role in core stability, bowel and bladder function, and intimate health. When this muscle group struggles after pregnancy and delivery, the effects extend well beyond what most people expect.
We’ll explore these often-overlooked signs and explain how pelvic floor physiotherapy supports comprehensive postpartum healing in Vancouver.
What Is the Pelvic Floor and Why Does It Matter After Pregnancy?
The pelvic floor consists of muscles, ligaments, and connective tissues that form a supportive sling at the base of your pelvis. These muscles support your bladder, uterus, and rectum while controlling urinary and bowel function. They also contribute to core stability and play an important role in intimate function.
During pregnancy, hormonal changes soften these tissues to prepare for delivery. The growing baby also places increasing pressure on the pelvic floor muscles. Delivery itself, whether vaginal or cesarean, creates additional stress on this muscle group. Research shows that these changes can persist well into the postpartum period, affecting various aspects of physical function.
The pelvic floor must regain strength, coordination, and endurance after these significant changes. When recovery is incomplete or complications arise, the effects reach beyond obvious symptoms like incontinence.
What Are the Hidden Signs of Pelvic Floor Impact After Pregnancy?
Many postpartum symptoms have connections to pelvic floor function that aren’t immediately obvious. These signs are often mistaken for typical recovery experiences or attributed to other causes.
Persistent Lower Back and Pelvic Discomfort
Ongoing lower back pain and pelvic discomfort often relate to pelvic floor dysfunction. When these muscles don’t function properly, your core stability suffers. Your body compensates by overusing other muscle groups, particularly in the lower back. This creates a cycle of tension and discomfort that extends beyond the pelvic region.
Unusual Vaginal Sensations
Feelings of heaviness, pressure, or fullness in the vaginal area signal potential pelvic organ prolapse or muscle tension issues. Some women describe a sensation that something is “falling out” or constant downward pressure. These symptoms often worsen with physical activity or prolonged standing.
Changes in Intimate Comfort
Pain during sexual activity, unusual sensitivity, or complete loss of sensation indicates pelvic floor involvement. These muscles directly affect intimate function, and dysfunction creates various uncomfortable symptoms. The emotional impact of these changes often compounds the physical challenges.
Bowel Function Difficulties
Constipation, incomplete bowel movements, or difficulty controlling bowel urgency all connect to pelvic floor function. These muscles coordinate with your anal sphincter and support proper elimination. When they’re not working well, bowel habits change significantly.
Subtle Urinary Changes
Beyond obvious leakage, watch for sudden strong urges, frequent nighttime urination, or difficulty starting urination. Some women experience minor leakage they dismiss as “just a few drops,” but these early signs often progress without proper attention.
How Does Pelvic Floor Physiotherapy Support Postpartum Recovery?
Pelvic floor physiotherapy involves specialized assessment and treatment techniques designed to restore proper muscle function. A qualified physiotherapist evaluates muscle strength, coordination, and endurance while identifying specific dysfunction patterns.
Treatment typically includes targeted exercises, manual techniques, and education about proper muscle activation. Studies indicate that structured pelvic floor rehabilitation can significantly improve various postpartum symptoms when implemented appropriately.
The approach is highly individualized because every woman’s experience differs. Some need to strengthen weak muscles, while others must learn to relax overly tense tissues. Proper assessment determines the most effective treatment strategy for your specific situation.
For women in Vancouver seeking comprehensive pelvic floor physiotherapy, specialized clinics offer evidence-based treatment approaches. These services focus on restoring function rather than simply managing symptoms.
What Lifestyle Strategies Support Pelvic Floor Recovery?
Several practical approaches support pelvic floor healing alongside professional treatment. These strategies help optimize your recovery environment and prevent further dysfunction.
Mindful Movement and Exercise
Gentle, progressive movement supports tissue healing and muscle function. Start with walking and basic core activation before advancing to more challenging activities. Avoid high-impact exercises until your pelvic floor regains adequate strength and coordination.
Healthy Bowel Habits
Maintaining regular bowel movements reduces strain on the pelvic floor. Include adequate fiber in your diet, stay well-hydrated, and avoid straining during elimination. Proper toilet posture with feet supported also reduces unnecessary pressure.
Smart Activity Modifications
Avoid heavy lifting and high-impact activities during early recovery. When you must lift objects, use proper body mechanics and engage your core muscles appropriately. Listen to your body and rest when symptoms worsen.
Stress Management
Physical and emotional stress affects muscle tension throughout your body, including the pelvic floor. Prioritize rest, seek support when needed, and practice stress-reduction techniques that work for you.
When Should You Consider Pelvic Floor Rehabilitation?
Don’t wait for symptoms to become severe before seeking professional assessment. Early intervention often prevents more complex problems and supports better long-term outcomes.
Consider pelvic floor evaluation if you experience any persistent symptoms beyond six weeks postpartum. This includes urinary or bowel changes, pelvic pain, intimate discomfort, or ongoing core weakness. Healthcare experts recommend early assessment for optimal recovery.
Even if you feel “mostly fine,” a postpartum pelvic floor check provides valuable information about your recovery progress. Many women benefit from preventive education and exercise instruction, even without obvious symptoms.
Professional assessment becomes particularly important if you’re planning future pregnancies or want to return to demanding physical activities. Understanding your current pelvic floor function helps guide safe activity progression and identifies areas needing attention.
Key Takeaways
- Pelvic floor dysfunction after pregnancy creates symptoms beyond urinary incontinence, including lower back pain, pelvic pressure, intimate discomfort, and bowel changes.
- The pelvic floor undergoes significant stress during pregnancy and delivery, and incomplete recovery affects core stability and overall function.
- Early recognition of subtle symptoms allows for more effective intervention and better long-term outcomes.
- Pelvic floor physiotherapy provides individualized assessment and treatment to restore proper muscle function through targeted exercises and manual techniques.
- Lifestyle modifications including mindful movement, healthy bowel habits, and activity modifications support natural healing processes.
- Professional evaluation is recommended for any persistent postpartum symptoms, even those considered “minor” or “normal.”
Don’t Let Pain Ruin Your Day
If you’re experiencing any concerning postpartum symptoms or want to ensure optimal recovery, consider connecting with a qualified pelvic floor physiotherapist. At Treloar Physiotherapy Clinic, we provide comprehensive pelvic floor assessments and personalized treatment plans designed to support your long-term physical well-being. Our patient-centered approach combines evidence-based techniques with the understanding and support you need during this important recovery period. Contact us to learn how we can help you rebuild strength, restore function, and return to the activities you love with confidence.
Frequently Asked Questions
What are common signs of pelvic floor dysfunction after pregnancy besides urinary issues?
Common signs include persistent lower back and pelvic pain, feelings of vaginal heaviness or pressure, pain during sexual activity, difficulty with bowel movements, and unexplained core weakness. These symptoms are often dismissed as normal postpartum changes but may indicate pelvic floor involvement requiring professional attention.
How soon after delivery can I start pelvic floor physiotherapy?
You typically start pelvic floor physiotherapy around 6-8 weeks postpartum, after your healthcare provider clears you for normal activities. However, gentle breathing and awareness exercises often begin much earlier. Some women benefit from assessment during pregnancy to prepare for postpartum recovery.
How does pelvic floor physiotherapy help with postpartum pain and mobility challenges?
Pelvic floor physiotherapy addresses muscle dysfunction that contributes to pain and mobility limitations. Treatment includes strengthening weak muscles, releasing tension in tight areas, improving coordination, and restoring proper movement patterns. This comprehensive approach often reduces pain and improves overall function beyond just pelvic symptoms.